Spondylolisthesis Physical Therapy Protocol: A Comprehensive Guide
This guide details a phased approach to rehabilitation, encompassing acute, subacute, and rehabilitation stages,
addressing pain, core stability, and functional restoration for optimal outcomes.
APTA resources and research emphasize early intervention,
while youth athlete protocols suggest varied timing for initiating physical therapy post-cessation of activity.
Non-operative treatment options, including physical therapy, are crucial,
with systematic reviews supporting their efficacy in managing spondylolysis and spondylolisthesis.
Understanding Spondylolisthesis
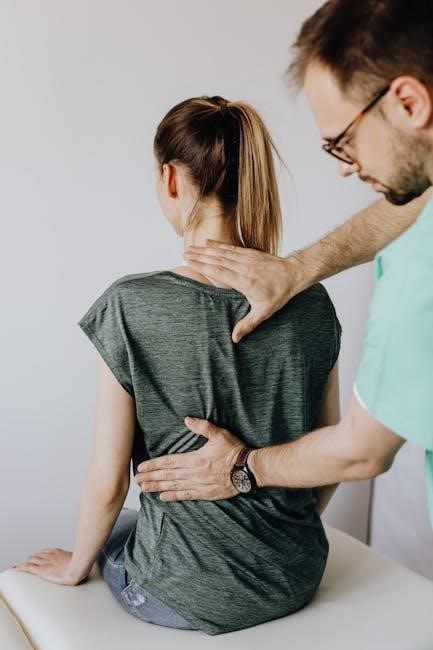
Spondylolisthesis, a condition characterized by the forward slippage of one vertebra over another, presents diverse clinical pictures. Degenerative lumbar spondylolisthesis, common in older adults, arises from age-related changes in the spine, often accompanied by spinal stenosis. Conversely, spondylolysis, frequently seen in youth athletes, involves a defect in the pars interarticularis.

Understanding the underlying cause is paramount for tailoring a physical therapy protocol. While some cases may be asymptomatic, others manifest as low back pain, radiating leg pain, or neurological deficits. The APTA provides guidance on diagnosing and managing these symptoms. Cessation of aggravating activities, particularly in young athletes, is often recommended, with varying opinions on the optimal timing for initiating rehabilitation.
Effective management necessitates a comprehensive understanding of the specific type of spondylolisthesis and its impact on the patient’s functional abilities.
Diagnosis and Classification
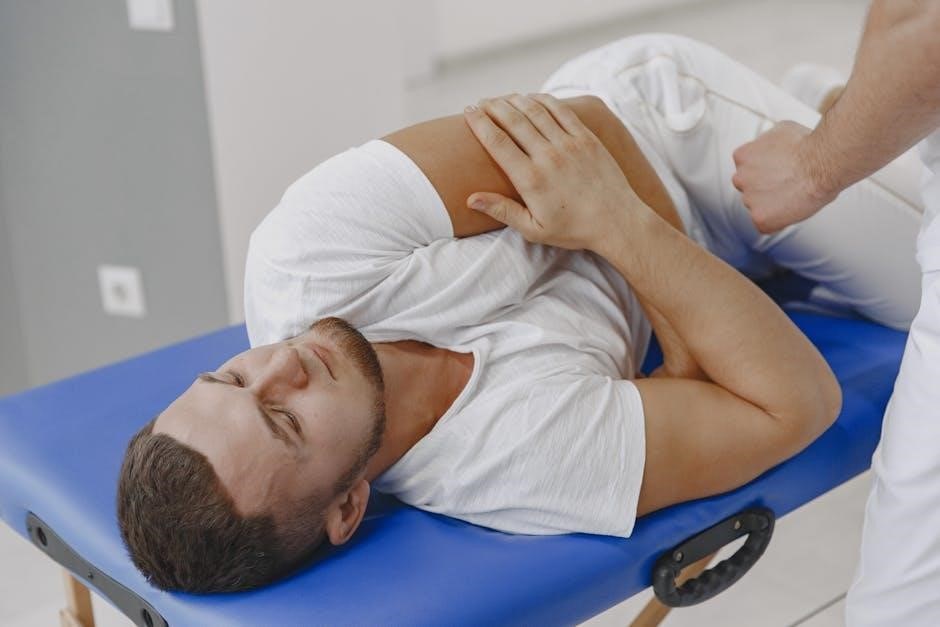
Accurate diagnosis of spondylolisthesis relies on a combination of patient history, physical examination, and imaging studies. Radiographic assessment, including X-rays, is crucial to visualize vertebral slippage and identify any associated defects. Classification systems, like the Meyerding classification, categorize the severity of slippage, guiding treatment decisions.
Distinguishing between different types – dysplastic, isthmic, degenerative, traumatic, or pathological – is essential. Degenerative lumbar spondylolisthesis often coexists with spinal stenosis, requiring a nuanced approach. The APTA emphasizes comprehensive assessment for accurate diagnosis.
Non-operative treatment eligibility is determined by factors like slippage degree, neurological involvement, and symptom severity. Systematic reviews highlight the importance of confirming the diagnosis before initiating any physical therapy intervention.
Goals of Physical Therapy

The primary goals of physical therapy for spondylolisthesis are to reduce pain, restore function, and prevent further progression of the condition. This involves a phased approach, starting with pain management and progressing to core stabilization and functional exercise.
Specific objectives include improving lumbar and pelvic mobility, enhancing neuromuscular control, and addressing any associated spinal stenosis components. For youth athletes, a key goal is facilitating a safe return to sport after a period of rest, as highlighted by rehabilitation considerations.
Long-term goals focus on patient education for self-management, promoting proper body mechanics, and preventing recurrence through ongoing exercise and activity modification.
Phase 1: Acute Phase (0-4 Weeks)
The initial phase (0-4 weeks) prioritizes pain and inflammation reduction. Rest from aggravating activities is paramount, potentially including a temporary cessation of sport for youth athletes – a minimum of three months is often recommended. Gentle range of motion exercises are introduced, avoiding movements that exacerbate symptoms.
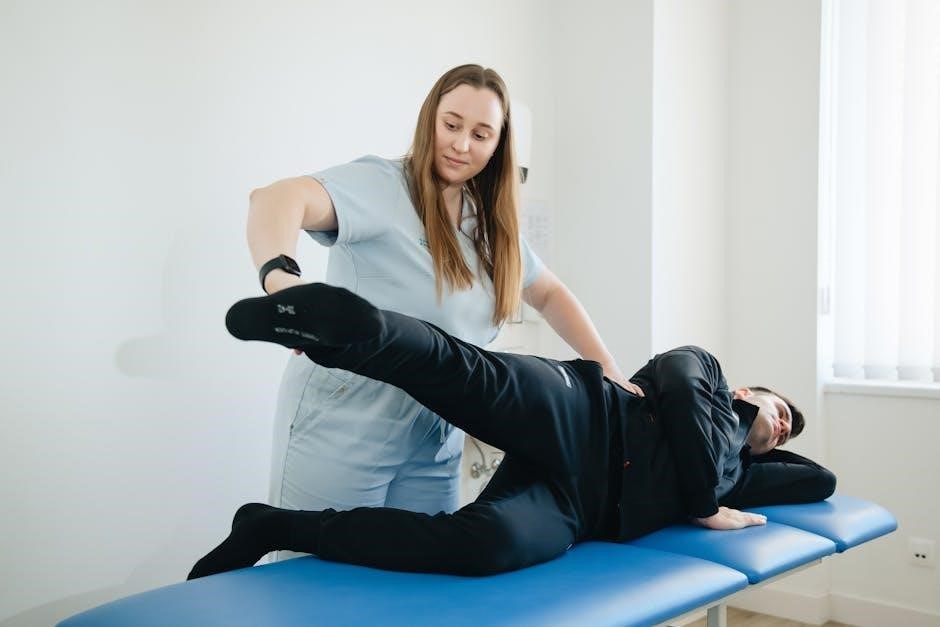
Focus is placed on patient education regarding proper posture and body mechanics. Initial core stabilization exercises are initiated, emphasizing gentle engagement of deep abdominal and back muscles. Modalities like heat or ice may be used for symptomatic relief, alongside activity modification.
The goal is to establish a baseline of pain control and prepare for more progressive exercises in subsequent phases.
Pain Management Strategies
Effective pain management is central to the initial stages of spondylolisthesis rehabilitation. Strategies include a combination of conservative approaches tailored to individual needs. Modalities such as heat and ice can provide symptomatic relief, reducing inflammation and muscle spasm. Careful activity modification, avoiding movements that provoke pain, is crucial.
Patient education regarding pain science and self-management techniques empowers individuals to actively participate in their recovery. Gentle range of motion exercises, performed within a pain-free range, help maintain joint mobility. Early core stabilization, focusing on deep muscle activation, provides support and reduces stress on the spine.
The aim is to establish a foundation for progressive exercise and functional restoration.
Core Stabilization Exercises ― Initial Focus
Initial core stabilization prioritizes activating deep abdominal and back muscles without exacerbating symptoms. Exercises begin with gentle engagement, focusing on maintaining a neutral spine. Transversus abdominis activation, often described as “drawing in” the belly button, is fundamental. Pelvic tilts and abdominal bracing are introduced to enhance core control.
These exercises are performed in supine, prone, and quadruped positions, progressing as tolerated. Emphasis is placed on proper form and controlled movements, avoiding lumbar extension or flexion. Breathing techniques are integrated to facilitate muscle activation and relaxation. The goal is to create a stable base of support for the spine.
Progression is guided by pain levels and functional improvements.
Activity Modification and Education
Patient education is paramount, explaining spondylolisthesis, its causes, and the importance of adherence to the rehabilitation program. Activity modification focuses on identifying and avoiding movements or postures that aggravate symptoms. This includes adjusting daily routines, work ergonomics, and recreational activities.
Guidance is provided on proper lifting techniques, maintaining good posture, and utilizing supportive devices if needed. Rest and cessation of aggravating activities, particularly in youth athletes, are emphasized for at least three months, potentially leading to favorable outcomes.
Understanding pain signals and respecting limitations are crucial for preventing re-injury. Self-management strategies, including home exercise programs and pain coping mechanisms, are taught to empower patients.
Phase 2: Subacute Phase (4-12 Weeks)
The subacute phase, spanning 4-12 weeks, focuses on progressively restoring function and building strength. Progressive core strengthening exercises are introduced, building upon the initial stabilization work, increasing intensity gradually. Lumbar and pelvic mobility exercises aim to improve range of motion and reduce stiffness, addressing any compensatory patterns.
Neuromuscular re-education is vital, retraining muscles to work efficiently and coordinating movements. Functional activities are incorporated, simulating daily tasks to bridge the gap between exercise and real-life demands.
Monitoring for symptom exacerbation is crucial, adjusting the program as needed. Early initiation of physical therapy, when symptoms resolve, may facilitate a quicker return to sport, as suggested by some research.
Progressive Core Strengthening
Progressive core strengthening builds upon the foundational stability achieved in Phase 1. Exercises evolve from static holds (planks, bridges) to dynamic movements, increasing challenge. Examples include bird-dogs, dead bugs with controlled limb movements, and side planks with hip dips.
Focus shifts to endurance and controlled motion, avoiding excessive lumbar flexion or rotation. Resistance can be added using light weights, resistance bands, or bodyweight variations. Proper form is paramount to prevent re-injury and ensure effective muscle engagement.
Integration of core work with functional movements prepares the patient for more demanding activities. APTA guidelines emphasize individualized programs, adapting to patient tolerance and progress.
Lumbar and Pelvic Mobility Exercises
Restoring optimal lumbar and pelvic mobility is crucial for reducing pain and improving function. Exercises target stiff joints and muscles, enhancing movement patterns. Gentle stretches like knee-to-chest, pelvic tilts, and cat-cow stretches are initially employed, focusing on pain-free range of motion.
Mobilization progresses to include dynamic movements, such as lumbar rotations and side bending. Pelvic tilts address imbalances and improve core control. Manual therapy, as guided by a physical therapist, may be incorporated to address specific joint restrictions.
Emphasis is placed on controlled movements, avoiding forceful or provocative positions. Individualized programs adapt to patient needs and tolerance, promoting gradual improvement in flexibility and stability.
Neuromuscular Re-education
Neuromuscular re-education focuses on restoring proper muscle activation patterns and coordination. Exercises aim to improve proprioception – the body’s awareness of its position in space – and enhance control of lumbar and pelvic muscles. Initial exercises involve conscious activation of deep core stabilizers, like the transverse abdominis and multifidus.
Progressive drills incorporate functional movements, challenging the patient to maintain stability while performing tasks like reaching, bending, and lifting. Biofeedback may be utilized to provide real-time feedback on muscle activity, aiding in correct movement patterns.
The goal is to retrain the nervous system to efficiently control spinal movement and prevent recurrence of symptoms, promoting long-term functional improvement.
Phase 3: Rehabilitation Phase (12+ Weeks)

The rehabilitation phase, extending beyond 12 weeks, centers on restoring full functional capacity and preparing for return to desired activities. Functional exercise progression involves dynamic movements mimicking real-life scenarios, like squatting, lunging, and twisting. Emphasis is placed on maintaining proper form and avoiding compensatory patterns.
For athletes, sport-specific training is integrated, gradually increasing intensity and complexity to simulate game conditions. Advanced core and stability training incorporates plyometrics and rotational exercises to enhance power and agility.
The focus shifts from pain management to optimizing performance and preventing re-injury, ensuring a safe and sustainable return to activity.
Functional Exercise Progression
This phase prioritizes translating strength and stability gains into real-world movements. Exercises begin with controlled, low-impact activities, gradually increasing in complexity and demand. Examples include walking programs progressing to jogging, step-ups, and controlled stair climbing.
Focus shifts to dynamic movements like squats, lunges, and reaching, emphasizing proper biomechanics and core engagement. Proprioceptive exercises, utilizing balance boards or unstable surfaces, enhance body awareness and control. Functional tasks, such as lifting and carrying, are introduced with appropriate modifications.
Progression is guided by symptom response and functional milestones, ensuring a safe and effective return to activity.
Sport-Specific Training (for Athletes)
This phase bridges rehabilitation and full athletic participation, reintroducing movements directly related to the athlete’s sport. Training begins with modified drills, focusing on technique and controlled loading. For example, a runner might start with short intervals, gradually increasing distance and speed.
Plyometric exercises, like jumping and bounding, are incorporated cautiously to enhance power and agility. Agility drills improve quickness and change-of-direction skills. Sport-specific conditioning builds endurance and prepares the athlete for the demands of competition.
Close monitoring of symptoms and biomechanics is crucial, with adjustments made to prevent re-injury. A gradual return to full participation is essential, guided by objective criteria.
Advanced Core and Stability Training
This stage focuses on refining core control and stability, progressing beyond basic exercises. Exercises include dynamic planks with perturbations, utilizing unstable surfaces like balance boards or foam rollers. Anti-rotation exercises challenge the core’s ability to resist twisting forces.
Functional movement patterns, mimicking athletic activities, are integrated. Examples include medicine ball throws, rotational lifts, and single-leg exercises with added resistance. Proprioceptive training enhances body awareness and joint position sense.
The goal is to achieve automatic core engagement during all movements, providing spinal support and preventing re-injury. This phase prepares the athlete for high-level activities and a return to sport.
Physical Therapy Techniques
Physical therapy employs a multifaceted approach to address spondylolisthesis. Manual therapy techniques, including soft tissue mobilization and joint mobilization, aim to restore optimal spinal mechanics and reduce muscle tension. Neuromuscular re-education focuses on retraining core muscles for proper activation and control.
Modalities like heat, ice, and electrical stimulation can be utilized for pain management and muscle relaxation. Therapeutic exercise forms the cornerstone of treatment, progressing from gentle core stabilization to advanced strengthening.
Patient education is crucial, emphasizing proper body mechanics and activity modification. A tailored program, guided by the APTA guidelines, ensures individualized care and optimal outcomes.
Manual Therapy Approaches
Manual therapy plays a vital role in spondylolisthesis treatment, focusing on restoring spinal alignment and reducing soft tissue restrictions. Techniques include gentle joint mobilization to improve lumbar and pelvic mobility, addressing any hypomobility contributing to pain. Soft tissue mobilization targets tight muscles, such as the paraspinals and hamstrings, releasing tension and improving flexibility.
Muscle energy techniques can be employed to correct muscle imbalances and restore proper biomechanics. Myofascial release addresses fascial restrictions impacting spinal movement.
These hands-on interventions, when combined with exercise, enhance treatment effectiveness and promote optimal spinal function, aiding in pain reduction and improved stability.
Modalities (e.g., Heat, Ice, Electrical Stimulation)
Adjunctive modalities can effectively manage pain and inflammation associated with spondylolisthesis. Cryotherapy (ice) is beneficial in the acute phase, reducing inflammation and muscle spasm. Heat therapy, applied later, promotes tissue relaxation and increases blood flow, easing muscle tension.
Electrical stimulation (e-stim), specifically neuromuscular electrical stimulation (NMES), aids in muscle re-education and strengthening of core stabilizers. Transcutaneous electrical nerve stimulation (TENS) can provide pain relief by modulating nerve signals.
These modalities are used strategically, complementing exercise and manual therapy, to optimize patient comfort and accelerate recovery, enhancing the overall rehabilitation process.
Non-Operative Treatment Considerations
Conservative management forms the cornerstone of treatment for many spondylolisthesis cases. Rest and activity modification are crucial initially, avoiding aggravating movements and activities. Physical therapy, as outlined in this protocol, plays a central role, focusing on core stabilization, lumbar mobility, and neuromuscular re-education.
Systematic reviews confirm the efficacy of non-operative approaches, including physical therapy, in alleviating pain and improving function. For youth athletes, a three-month cessation of sport is often recommended, with varying opinions on the optimal timing for initiating rehabilitation.
Careful monitoring of symptoms and functional progress guides treatment adjustments, aiming to optimize outcomes and prevent the need for surgical intervention.
Rest and Cessation of Aggravating Activities
Initial management frequently involves a period of relative rest, not complete inactivity, to reduce inflammation and pain. Identifying and avoiding activities that exacerbate symptoms is paramount; this includes specific movements, prolonged sitting, or heavy lifting. For young athletes, a minimum of three months of cessation from sport is often prescribed, demonstrating a strong correlation with favorable clinical outcomes.
This period of rest allows tissues to heal and prepares the patient for a progressive rehabilitation program. However, prolonged inactivity can lead to deconditioning, emphasizing the importance of a timely return to appropriate activity under the guidance of a physical therapist.
Careful self-monitoring of pain levels during and after activity is essential.
Importance of Early vs. Delayed Physical Therapy
The timing of physical therapy initiation remains a debated topic, particularly in youth athletes with spondylolysis. Some protocols advocate for early intervention, commencing once initial pain subsides, aiming for quicker return to sport. Conversely, others recommend a more conservative approach, delaying therapy until after a three-month period of complete rest.
Research suggests that initiating physical therapy sooner may facilitate an earlier return to activity compared to delayed intervention. However, this must be carefully considered on an individual basis, factoring in symptom severity and patient compliance. A tailored approach, guided by a physical therapist, is crucial for optimizing outcomes.
Early intervention focuses on pain management and core stabilization.
Degenerative Lumbar Spondylolisthesis Specifics
Degenerative lumbar spondylolisthesis often presents alongside spinal stenosis, necessitating a comprehensive physical therapy approach. Treatment focuses on addressing both the instability and the neurogenic claudication symptoms – pain, numbness, or weakness in the legs. APTA guidelines emphasize individualized programs tailored to symptom presentation.
Physical therapy interventions prioritize improving lumbar and pelvic mobility, strengthening core musculature, and enhancing neuromuscular control. Specific exercises aim to reduce pressure on neural structures and improve functional capacity. Modalities like heat, ice, or electrical stimulation may provide short-term pain relief.
Management also includes patient education on activity modification and postural correction.
Addressing Spinal Stenosis Components
Spinal stenosis, frequently coexisting with degenerative spondylolisthesis, demands targeted physical therapy. Interventions aim to maximize the spinal canal space and alleviate nerve compression symptoms – often leg pain and neurogenic claudication. Key strategies involve extension-based exercises, promoting lumbar lordosis and reducing canal narrowing.
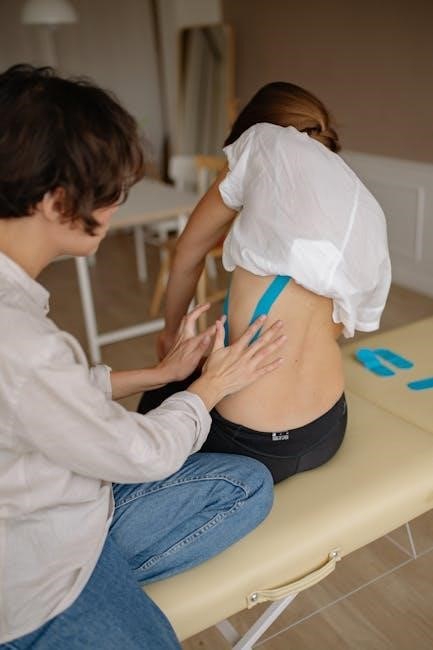
Flexion-based exercises, while sometimes helpful, require careful monitoring to avoid exacerbating instability. Core stabilization is paramount, enhancing spinal support and reducing stress on affected segments. Neuromuscular re-education improves movement patterns and reduces compensatory strategies.
APTA resources highlight the importance of a comprehensive assessment and individualized treatment plans.
APTA Guidelines and Recommendations
The American Physical Therapy Association (APTA) provides crucial guidance for managing degenerative lumbar spondylolisthesis and associated spinal stenosis. Recommendations emphasize a patient-centered approach, focusing on minimizing pain, improving function, and preventing disability. Evidence-based practice dictates utilizing a combination of exercise, manual therapy, and patient education.
APTA resources advocate for thorough assessments to identify specific impairments and tailor interventions accordingly. Guidelines support progressive loading of the spine, promoting core stability, and addressing neuromuscular deficits. Membership unlocks access to detailed clinical practice guidelines and research updates.
Adherence to these recommendations ensures optimal patient outcomes and safe, effective care.
Monitoring Progress and Preventing Recurrence
Regular assessment is vital throughout the spondylolisthesis rehabilitation process. Monitoring includes pain levels, functional limitations, and core muscle strength. Objective measures, like range of motion and functional movement screens, track progress effectively. Patient reported outcomes provide valuable insight into perceived improvement.
Preventing recurrence necessitates a long-term commitment to core stabilization and postural control. Continued exercise, even after discharge, maintains strength and stability. Activity modification avoids re-aggravation of symptoms. Education empowers patients to self-manage their condition.
Consistent follow-up ensures adherence and addresses any emerging issues promptly.
Patient Education for Long-Term Management
Comprehensive education is paramount for successful long-term management of spondylolisthesis. Patients must understand their condition, including anatomical factors and biomechanical implications. Proper body mechanics during daily activities, like lifting and bending, are crucial to minimize stress on the spine.
A home exercise program, tailored to individual needs, reinforces core stability and flexibility. Awareness of aggravating activities allows for proactive modification. Maintaining a healthy weight reduces spinal load. Ergonomic adjustments at work and home support optimal posture.
Recognizing warning signs of symptom recurrence enables timely intervention.
Return to Activity Criteria
A gradual return to activity is essential, guided by symptom response and functional milestones. Pain levels should be minimal, ideally below 2/10, during and after activity. Full, pain-free range of motion in the lumbar spine and hips is required. Demonstrated core stability, evidenced by successful completion of advanced exercises, is critical.
Functional tasks, such as walking, stair climbing, and lifting, must be performed without exacerbating symptoms. For athletes, sport-specific movements should be introduced progressively, starting with low-impact drills. A three-month cessation of sport is often recommended initially, followed by a phased return.
Successful completion of a functional capacity evaluation may be beneficial.
